If you are a parent trying to understand whether insurance covers ABA therapy in Georgia, the short answer is yes, many plans do. But the full answer depends on the type of insurance you have, your child’s diagnosis, medical necessity, and whether the provider is in network. That is where many families get stuck.
The process can feel confusing at first because parents often hear different answers from different people. One family may be told ABA is covered, while another is told more paperwork is needed or that their plan works differently. In Georgia, coverage is often available, but the details matter.
Understanding how ABA coverage works can help you avoid delays, ask better questions, and move toward services with more confidence. Whether you are just starting the diagnostic process or already looking for a provider, it helps to know what insurance typically covers and what to check before therapy begins.
The Short Answer: Yes, ABA Therapy Is Often Covered In Georgia
ABA therapy is often covered in Georgia through many private insurance plans and through Medicaid for eligible children. For many families, that is encouraging news. Still, coverage is not automatic in every case, and it is not exactly the same from one plan to another.
Some plans are required to include autism-related treatment benefits, including ABA therapy, while others may follow different rules. Even when ABA is covered, families may still need to meet plan requirements such as getting an autism diagnosis, confirming medical necessity, and obtaining prior authorization before services begin.
That is why it is important not to stop at a general yes or no. The better question is whether your specific plan covers ABA therapy for your child’s needs and what steps are required to access those benefits.
What Ava’s Law Means For ABA Therapy Coverage In Georgia
A major reason many Georgia families are able to access ABA therapy through insurance is Ava’s Law. This law helped expand access to autism treatment by requiring many state-regulated health plans to provide coverage for autism-related services, including Applied Behavior Analysis.
For parents, this matters because it created a stronger path to medically necessary autism care. Instead of treating ABA therapy as something optional or separate, many plans must recognize it as part of covered treatment for children who meet the criteria.
At the same time, Ava’s Law does not mean every health plan works the same way. The law generally applies to state-regulated insurance plans, which is why some families still run into confusion when they call their insurance company. The key is knowing that Georgia has a framework for autism coverage, but your exact benefits still depend on your policy.
Which Insurance Plans May Cover ABA Therapy In Georgia
One of the most important details is the difference between fully insured plans and self-funded employer plans. This distinction can affect whether Georgia’s insurance rules apply directly to your coverage.
If your family has a fully insured private plan regulated by the state, there is a stronger chance that ABA therapy falls under the autism treatment benefits required in Georgia. These plans are often the ones parents are referring to when they say insurance covers ABA therapy.
Self-funded employer plans are different. These plans are often funded by the employer rather than regulated in the same way as standard state insurance plans. Because of that, they may not have to follow the same Georgia-specific requirements. That is one of the biggest reasons families can get different answers even when they both have commercial insurance.
Medicaid is another important pathway. For many eligible children in Georgia, Medicaid can cover ABA therapy when the proper criteria are met. For some families, Medicaid may be the most direct route to services. For others, private insurance may be primary. In some situations, families may need help understanding how both work together.
Does Georgia Medicaid Cover ABA Therapy?
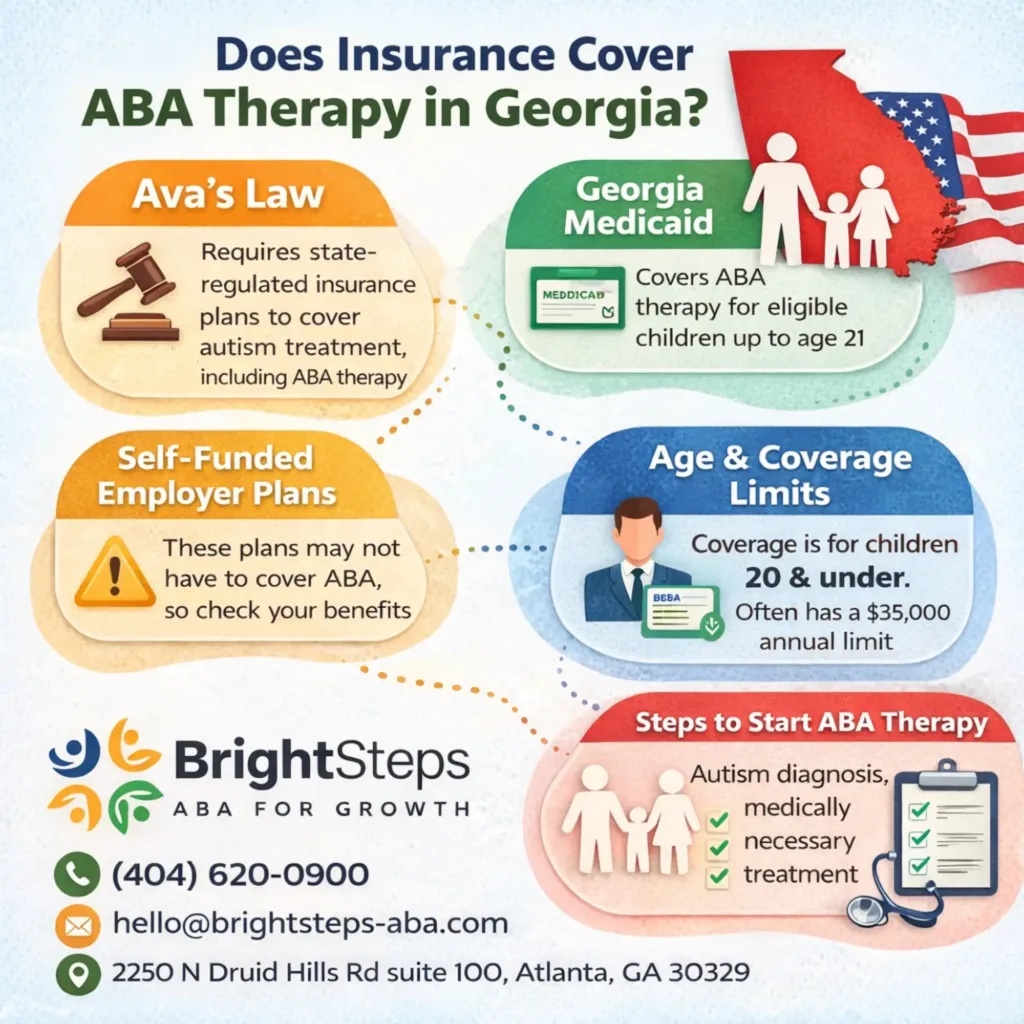
Yes, Georgia Medicaid can cover ABA therapy for eligible children. This is an important point because many parents specifically search for Medicaid coverage when they are trying to understand what services their child can receive after an autism diagnosis.
Medicaid coverage usually depends on medical necessity and required documentation. That often includes a formal autism spectrum disorder diagnosis, clinical recommendations, and approval steps that show the treatment is appropriate for the child’s needs. Even when Medicaid covers ABA therapy, families may still need to work through authorizations and provider availability.
This is why Medicaid coverage should not be viewed as a simple yes with no next steps. It is better to think of it as a real coverage path that still requires the right evaluation, records, and care coordination. For families who qualify, it can play a major role in making ABA services accessible.
What Insurance Usually Requires Before ABA Therapy Starts
Even when insurance covers ABA therapy, there are usually conditions that have to be met before services begin. The first is often a documented autism diagnosis. In most cases, insurance companies want clear clinical documentation that the child has been diagnosed with autism spectrum disorder.
The next step is medical necessity. This means the treatment must be shown as appropriate and necessary for the child’s functioning, development, and daily needs. Insurance companies often review evaluations and treatment recommendations to decide whether they will approve care.
Prior authorization is another common requirement. This means insurance may need to approve the treatment plan before sessions start or before a certain number of hours are provided. Families sometimes discover ABA is technically covered but still delayed because authorization was not completed yet.
Network status also matters. If a provider is in network, coverage may be smoother and out-of-pocket costs may be lower. If the provider is out of network, families may face higher costs or different reimbursement rules. This is why insurance verification is one of the most important early steps.
Why Some Families Still Get Confusing Answers
One of the hardest parts of this process is that families may hear yes from one source and no from another. That does not always mean someone is giving wrong information. Sometimes it means the situation depends on details that were not explained clearly.
For example, one child may qualify under a state-regulated private plan, while another family may have a self-funded employer plan with different rules. One policy may require prior authorization before care begins, while another may need additional documentation about treatment hours or provider credentials.
Families may also run into issues if they call insurance before all records are in place. A parent might ask if ABA is covered and get a vague answer because the representative cannot confirm benefits without diagnosis details, billing codes, or provider information. That uncertainty can feel frustrating, especially when families are eager to begin services.
This is why it helps to ask more specific questions instead of only asking whether ABA therapy is covered. A better conversation includes questions about diagnosis requirements, authorization steps, in-network providers, and out-of-pocket costs.
What Costs Families May Still Pay
Insurance coverage does not always mean therapy is free. Depending on the plan, families may still be responsible for deductibles, copays, coinsurance, or other out-of-pocket costs. These costs can vary widely from one policy to another.
Some families have plans with strong coverage but still need to meet a deductible before benefits fully apply. Others may owe a copay for each visit or a percentage of the allowed cost. If a provider is out of network, those costs may be higher.
It is also important to ask whether there are limits related to authorizations or approved treatment periods. Even when coverage exists, the insurer may review progress and continue authorizing care in stages rather than approving everything at once. Knowing this early can help families plan financially and avoid surprises.
How To Check Whether Your Child’s ABA Therapy Is Covered
The best place to start is with your insurance plan details. Find out whether your plan is fully insured, self-funded, Medicaid, or another type of coverage. That single detail often shapes the rest of the conversation.
Next, ask whether ABA therapy for autism spectrum disorder is a covered benefit under your child’s plan. Be direct and specific. General questions sometimes lead to general answers, so it helps to mention autism treatment and ABA by name.
Then ask about prior authorization, diagnosis requirements, and whether an in-network provider is required. You should also ask what your expected out-of-pocket costs would be. That includes deductibles, copays, coinsurance, and any coverage limitations tied to authorization periods.
Many families also benefit from working with a provider who helps verify benefits and explain next steps. That support can make the process feel more manageable and reduce the guesswork that often slows families down.
BrightSteps ABA supports families across the Atlanta area with compassionate, individualized care and a family-centered approach. For parents who are trying to understand the next step after diagnosis or sort through insurance questions before starting services, having a provider that values clear communication can make the process feel much less overwhelming.
Questions To Ask Your Insurance Company
When you call your insurance company, the goal is not just to hear that ABA is covered. The goal is to get clear, useful details about how coverage works under your specific plan.
Ask whether ABA therapy is covered for a child with an autism diagnosis. Ask whether your plan is fully insured or self-funded. Ask if prior authorization is required, whether the provider must be in network, and what your financial responsibility will be.
You should also ask if coverage depends on a treatment plan review, progress updates, or reauthorization after a set number of hours or months. These details can affect how quickly your child starts care and what you should expect once services are underway.
Moving Forward With More Confidence
So, does insurance cover ABA therapy in Georgia? In many cases, yes. Georgia families often have access to ABA coverage through private insurance or Medicaid, especially when the child has a documented autism diagnosis and the treatment is medically necessary.
The part that causes confusion is not usually whether ABA can be covered. It is understanding which plans apply, what documentation is needed, and how to move through the approval process without unnecessary delays. That is why early insurance verification matters so much.
If you are starting this process now, focus on getting clear answers about your specific plan. Once you know how your insurance works, you can make more informed choices about providers, costs, and the path to services. For families in Georgia, that clarity can make the first steps toward ABA therapy feel much more manageable.
FAQs
Does Insurance Cover ABA Therapy In Georgia?
Yes, many insurance plans in Georgia cover ABA therapy, especially for children with autism spectrum disorder. Coverage depends on the type of plan, medical necessity, and plan requirements.
Does Georgia Medicaid Cover ABA Therapy?
Yes, Georgia Medicaid can cover ABA therapy for eligible children. Families usually need a qualifying diagnosis, supporting documentation, and any required authorization.
Do All Insurance Plans In Georgia Have To Cover ABA Therapy?
No. Many state-regulated plans may cover ABA therapy, but self-funded employer plans can work under different rules. That is why coverage varies from one family to another.
Do You Need An Autism Diagnosis For Insurance To Cover ABA Therapy?
In most cases, yes. Insurance usually requires a documented autism diagnosis along with evidence that ABA therapy is medically necessary.
Is Prior Authorization Required For ABA Therapy?
Often, yes. Many plans require prior authorization before ABA services begin or before a treatment plan is approved for ongoing care.
Will Families Still Have Out-Of-Pocket Costs?
Possibly. Depending on the plan, families may still pay deductibles, copays, coinsurance, or higher costs for out-of-network care.
What If My Insurance Says No?
A denial does not always mean the end of the process. Sometimes more documentation, a corrected authorization request, or a formal appeal may help move the case forward.


